An Israeli startup is working on an injection that could both prevent and treat acute radiation poisoning at nuclear disaster sites, using stem cells from placenta donated by women after giving birth.
Israeli biopharma company Pluri, which is developing the jab, says it could potentially be administered to first responders following a nuclear meltdown, mitigating the deadly effects of radiation exposure even before they arrive at the site.
Exposure to high levels of radiation can harm a person’s ability to produce red and white blood cells and platelets – the key ingredients for the body to heal itself – and impair organ function.
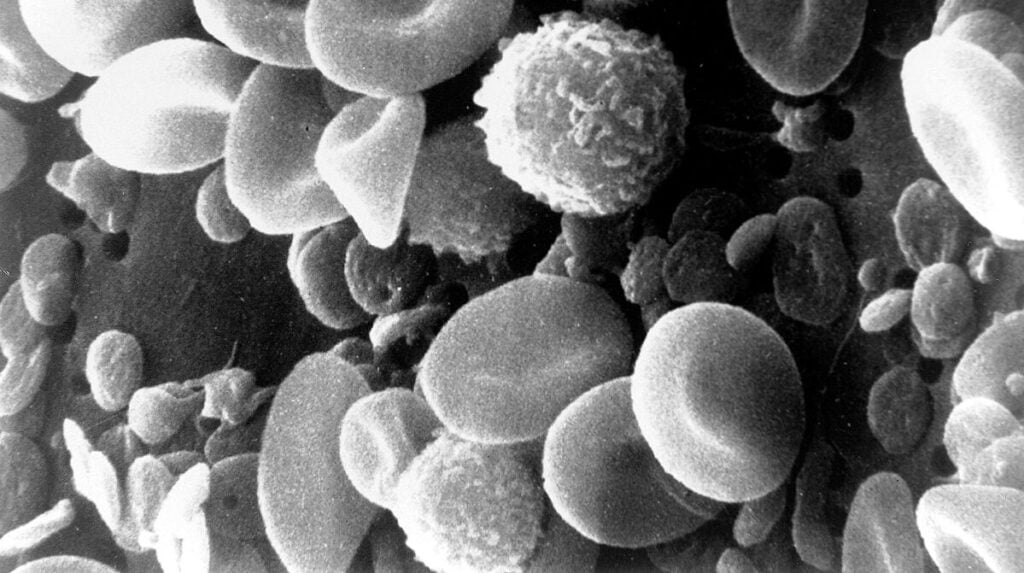
The stem cells that form the basis of the Pluri injection, however, boost the production of white and red blood cells and platelets, creating an optimum environment for recovery from the radiation exposure.
“Once the cells are injected into the muscle, they start to sense the environment, and respond by providing the body with the building blocks it needs in order to recover,” Yaky Yanay, CEO and president of Pluri, tells NoCamels.
Initial studies of the injection found that animals exposed to radiation and then given the jab were over three times more likely to survive than the animals who did not receive the treatment after exposure.
Furthermore, animals dosed prior to radiation exposure were 18 times more likely to survive, the researchers found.
Each vial created by Pluri can contain up to 100 million stem cells. According to the company, all the physician needs to do is inject them into the patient.
Miracle Cells
Stem cells have unique properties that make them ideal for use in medical treatments. Not only do they have the ability to change form and function (known as cellular differentiation), they can also inhibit tumor growth, enhance or suppress the performance of the immune system (known as immunomodulation) and repair damaged tissue.
Pluri’s treatment is created by placing the stem cells inside bioreactors – tanks that provide an ideal environment for them to proliferate and that can grow up to 40 billion cells at a time.
The cells are “fed” a liquid rich in glucose, amino acids and other substances in order to remain healthy.

Pluri also promotes cell proliferation by imitating the most suitable environment for placenta cells: the human body. They do this by tweaking factors in the bioreactor such as temperature, pH and the combination of gases present.
“The idea behind our technology was to build a system that mimics the human body – the most complicated, amazing control system – because we believe that it is the ideal way to grow cells,” says Yanay.
“What we learned is that these systems are extremely efficient for cell growth. It’s actually so efficient that from a single placenta, we can get enough cells to treat more than 20,000 patients.”
The placentas are only donated by women who experience full-term delivery. Yanay calls this a “very straightforward process,” which has already been approved by the US Food & Drug Administration, the European Medicines Agency and the Pharmaceutical Division of Israel’s Ministry of Health.
Sign up for our free weekly newsletter
Subscribe
Stem cells found in placenta have been shown to improve the quality of life for patients with spinal cord injuries or multiple sclerosis, among other disorders.
Pluri is now proving that the cells may have a similar impact on radiation poisoning.
Radiation harms a cell’s DNA, causing it to prevent reproduction, explains Pluri’s Chief Medical Officer Dr. Nitsan Halevy. This means that the body does not create enough red and white blood cells and platelets – among other cells – to remain healthy.
“This is the acute damage that radiation does,” she says.
A New Mission
Pluri has been treating various conditions with its cell treatment since 2001, including muscle regeneration for patients following hip fracture surgery and Graft-Versus-Host Disease – when the immune cells of transplanted tissue attack a patient’s own tissues.
It was only after witnessing the 2011 Fukushima nuclear disaster in Japan that the company thought to apply its technology to radiation poisoning.

“We saw that nuclear meltdown is something that can happen anywhere,” says Yanay. “That time it was Japan, but Europe is full of very old reactors too.”
After a discussion with a hematologist at Hadassah Medical Center in Jerusalem, the team learned that placenta-derived stem cells were suitable for radiation treatment.
At present, there are no other treatments for radiation poisoning that use stem cells taken from a placenta.
And while the two primary treatments in existence both – like Pluri – encourage the production of white blood cells, the company says its cell-based treatment is unique as it also stimulates the production of platelets and red blood cells.
The Haifa-based firm has signed a three-year, $4.2 million contract with the US National Institute of Allergy and Infectious Diseases to further develop its treatment.
Pluri hopes that the contract will ultimately lead to the purchase of the therapy by the US Strategic National Stockpile – the country’s repository of critical medical supplies – as a countermeasure for radiation exposure.
“Life on Earth begins and ends with cells,” says Yanay. “Our job is to explore and to use the power of this microscopic universe to create products that support the wellbeing of humanity.”
Related posts

Israeli Medical Technologies That Could Change The World

Harnessing Our Own Bodies For Side Effect-Free Weight Loss

Missing Protein Could Unlock Treatment For Aggressive Lung Cancer




Facebook comments