An Israeli man regained his sight after a decade of blindness following the first artificial cornea implantation developed by Israeli medical tech company CorNeat Vision, the company announced this month.
The patient, Jamal Furani, a resident of Haifa, began suffering some vision loss 10 years ago due to edema and other background diseases that damaged his corneas, and became bilaterally blind. This month, the 78-year-old became the first person in the world to be successfully implanted with CorNeat’s synthetic cornea, the CorNeat KPro, after the startup received the go-ahead last summer for human implantation.
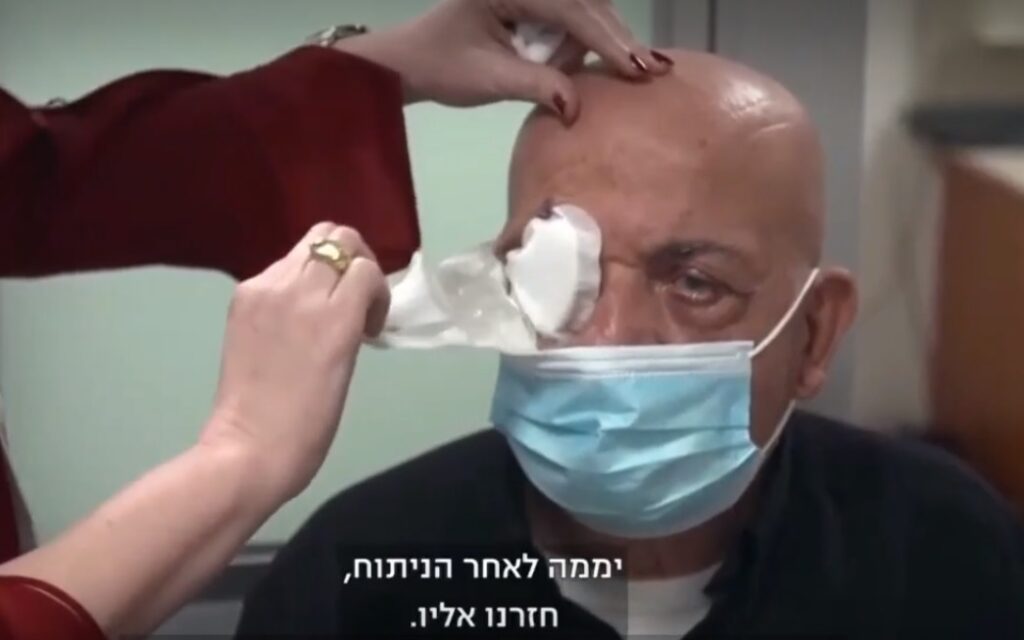
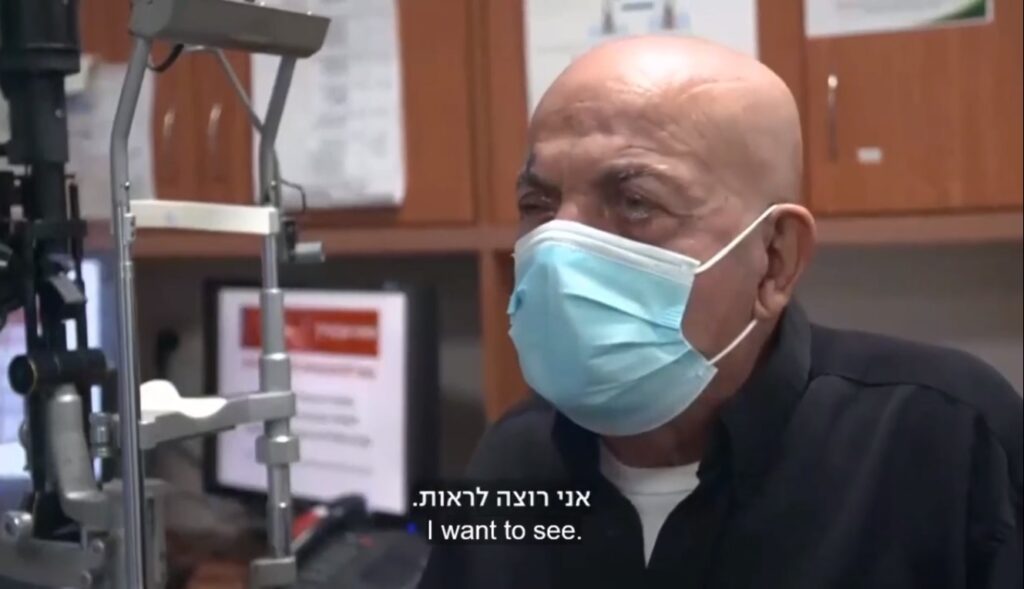
The procedure was performed recently by Professor Irit Bahar, director of the Ophthalmology Department at the Rabin Medical Center (also known as Beilinson Hospital). CorNeat said that the patient was able to immediately read a text and see family members after the bandages were removed.
SEE ALSO: Israeli Medtech Startup CorNeat Vision Uses Patented Implants To Treat Blinding Diseases
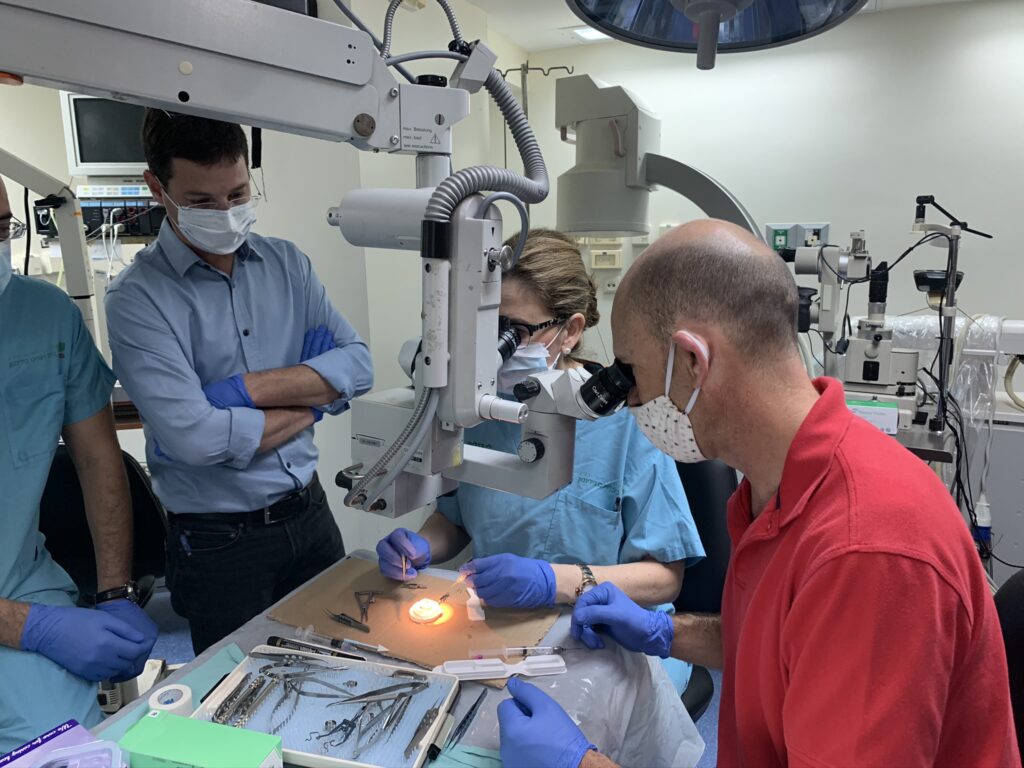
“The surgical procedure was straightforward and the result exceeded all of our expectations,” Professor Bahar said in a statement. “The moment we took off the bandages was an emotional and significant moment. Moments like these are the fulfillment of our calling as doctors. We are proud of being at the forefront of this exciting and meaningful project which will undoubtedly impact the lives of millions.”
CorNeat Co-Founder and Chief Medical Officer Dr. Gilad Litvin, the inventor of the CorNeat KPro, said the experience was “surreal.”
“After years of hard work, seeing a colleague implant the CorNeat KPro with ease and witnessing a fellow human being regain his sight the following day was electrifying and emotionally moving, there were a lot of tears in the room,” Dr. Litvin emphasized.
He hailed the surgery as “an extremely important milestone for CorNeat Vision” and a “key in our journey to enable people around the world to fully enjoy their vision potential.”
The Israeli patient was one of 10 people approved for a trial with CorNeat’s implants at the Rabin Medical Center, with two additional sites planned to open this month in Canada and six others at different stages in the approval process in France, the US, and the Netherlands, said Almog Aley-Raz, CorNeat Vision’s co-founder, CEO and VP R&D.
This first trial includes blind patients who are not suitable candidates for – or have failed – one or more corneal transplantations.
“Given the exceptional visual performance of our device, the expected healing time and retention, and the fact that it cannot carry disease, we plan to initiate a second study later this year with broader indications to approve our artificial cornea as a first-line treatment, displacing the use of donor tissue used in full-thickness corneal transplantations,” said Aley-Raz.
He added that the CorNeat KPro’s first-in-human implantation is the first step in a multi-national clinical trial toward attaining a CE mark, FDA clearance, and China NMPA approval.
CorNeat’s innovative ophthalmic solutions
Founded in 2015 and based in Ra’anana, CorNeat offers a few innovative solutions including the CorNeat KPro, and the CorNeat EverPatch, an artificial connective tissue substitute.
The CorNeat KPro implant is designed to replace deformed, scarred or opacified corneas and aims to fully rehabilitate the vision of corneally blind patients. The CorNeat KPro’s lens integrates with resident ocular tissue using a patented synthetic non-degradable nano-fabric placed under the conjunctiva (the tissue that lines the inside of the eyelid).

Current biological solutions are either sutured to or become integrated with native corneal tissue, which lacks blood vessels and heals poorly, Dr. Litvin told NoCamels in an interview in September.
“The holistic statement that we have as a company is to attempt to give back sight to people who are blind, to cure ophthalmic disease in that fashion, [and] try to bring more quality of life, greater equality and sustainability to our societies worldwide,” he said.
“Some of the indications that cause blindness, specifically corneal blindness, are more prevalent in less privileged areas, and it’s our mission to make profits but also to support these areas in the world as well,” Dr. Litvin added.
“The challenge [of this technology] is to embed this artificial material within our own tissue, and we know that any foreign body that goes into our body, usually the body tries to push it out or encapsulate it,” Litvin explained.
Sign up for our free weekly newsletter
SubscribeCorNeat KPro snaps into the patient’s trephined cornea and is then sutured to the eye using three non-degradable sutures, which reduces risk and minimizes the time the eye is trephined and open to less than one minute. The KPro lens enables post-operative ophthalmic examinations and subsequent surgeries like cataract surgery. Additionally, the KPro cannot carry any infectious agent including COVID-19.

“We wanted to create a device that doesn’t need any tissue, if you could have a completely synthetic alternative to the human donor tissue,” Litvin said. “The second target was to create a procedure that would be simple to perform, something that would be simple to teach and would create a feeling of self-confidence in our surgeons when they attempt to perform this for the first time and later on.”
CorNeat’s patented implants utilize advanced cell technology and nanoscale chemical engineering to mimic the structure and function of cellular and subcellular structures, which stimulates cellular growth and facilitates complete integration with surrounding tissue.
Corneal blindness
According to the World Health Organization, approximately two million new cases of corneal blindness are reported each year, and 30 million people worldwide are legally blind in one or both eyes from corneal injury and disease.
A recent study published JAMA Ophthalmology found that the shortage of corneas is around one available cornea for 70 needed. In China, some two million patients wait for keratoplasty (corneal transplantation) every year and only a few thousand transplants are available.
“If we look around the world there are about 55 percent of the world population that has no accessibility at all to corneal tissue,” Dr. Litvin told NoCamels. “Every year, the number grows because of this bottleneck created by the gap between the number of people who become blind and the number of people who are treated.”
Litvin also noted how, in order to properly transplant corneas, ophthalmologists must specialize in corneal transplantation, a procedure that takes at least a year or two to learn. Additionally, once a cornea is harvested, ophthalmologists have only one week to implant it, whereas CorNeat’s technology has a shelf life of two years.
Glaucoma solution
CorNeat is also set to begin trials for the CorNeat EverPatch, the first synthetic and non-degradable tissue substitute for ophthalmic surgeries. The EverPatch replaces the use of human tissue and degradable collagen patches for covering and concealing implants like glaucoma drainage devices and for mending traumatic breaks.
The EverPatch is composed of a non-woven, polymer matrix that imitates the extracellular matrix, stimulating cellular colonization and integration with the surrounding tissue.
According to Litvin, irreparable damage to the eye’s integrity makes direct and immediate closure impossible, which makes patching the area with preserved and processed tissue the only treatment option.

In addition to the EverPatch, CorNeat has also developed the eShunt, a solution for those who suffer from glaucoma. Glaucoma is a disease of the eye’s optic nerve that occurs when fluid pressure builds up in the anterior chamber of the eye as a result of excess fluid, or the aqueous humor. The eShunt works to regulate intraocular pressure while addressing the shortcomings of alternatives like laser surgery, incisional surgery, and glaucoma drainage devices.
SEE ALSO: Israeli Startup’s Synthetic Cornea Approved for First Human Implantation
“Glaucoma currently lacks a very efficient solution either surgical or medical. All solutions are only partial and give only some form of pressure-lowering effect but not comprehensive enough,” Dr. Litvin said.
The eShunt has successfully passed initial bench tests and animal trials demonstrating seamless integration and an efficient procedure taking less than ten minutes, and the R&D and preclinical phases are expected to take 12-15 months, Dr. Litvin indicated at the time.
CorNeat has registered five patents on its technology, including one in dental medicine, an area that also relies heavily on tissue substitutes.
Noah Sheidlower contributed to this report.
Related posts
Editors’ & Readers’ Choice: 10 Favorite NoCamels Articles

Forward Facing: What Does The Future Hold For Israeli High-Tech?

Impact Innovation: Israeli Startups That Could Shape Our Future



Facebook comments