To the reasons why chemotherapy sometimes does not work, we can now add one more: bacteria.
In a study published recently in the prestigious journal Science, Israeli researchers have found that certain bacteria can be found inside human pancreatic tumors. Some of these bacteria contain an enzyme that inactivates a common drug used to treat various cancers, including pancreatic cancer.
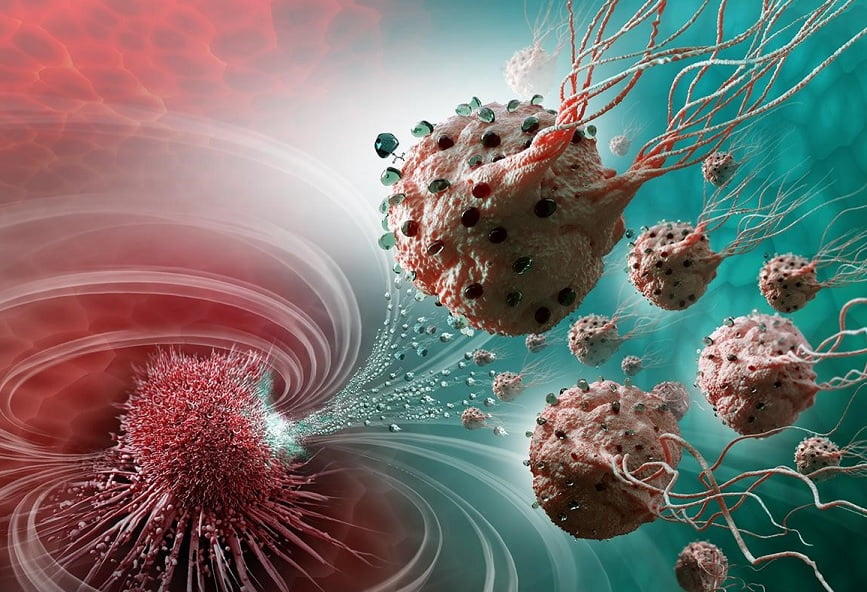
In the experiment, mice were used to demonstrate how treatment with antibiotics, on top of chemotherapy, may be significantly superior to treatment with chemotherapy alone.
SEE ALSO: Researchers Find Why Leukemia Recurs After Successful Chemotherapy
According to Weizmann Institute’s Dr. Ravid Straussman,”we first used different methods to prove that there really were bacteria inside the tumors. Then, we decided to look at the effect that these bacteria might have on chemotherapy.”
The researchers isolated bacteria from the tumors of pancreatic cancer patients and tested how they affect the sensitivity of pancreatic cancer cells to gemcitabine, a chemotherapy drug. Indeed, some of those bacteria kept the drug from working. Further investigation showed that these bacteria metabolize the drug, making it ineffective.
The researchers were able to find the bacterial gene responsible for this, a gene called cytidine deaminase (CDD). They demonstrated that CDD comes in two forms – a long and a short form. Only bacteria with the long form of the CDD gene could inactivate gemcitabine. The drug had no apparent effect on the bacteria.
A mechanism that inactivates drugs
The research team examined over 100 human pancreatic tumors to show that these particular bacteria with long CDD do live in the patient’s pancreatic tumors. They also used multiple methods to visualize the bacteria inside human pancreatic tumors. This is crucial, since bacterial contamination is a real issue for lab studies.
Sign up for our free weekly newsletter
SubscribeOddly enough, it was an earlier incidence of bacterial contamination that led Straussman and his team to this present study. They had been looking for evidence that normal cells in the cancer’s environment contribute to chemotherapy resistance. While testing the effect of many normal, non-cancerous, human cells on the sensitivity of cancer cells to chemotherapy, they found a specific sample of normal human skin cells that rendered pancreatic cancer cells resistant to gemcitabine.
Tracking down the cause led the team to bacteria that had accidentally contaminated these skin cells. “We nearly threw it away,” says Straussman, “but then we decided to follow it up, instead.” After revealing how these bacteria degraded the drug, he began to wonder if other bacteria might have a similar mechanism for inactivating the drug, and whether such bacteria might be found inside human tumors.
In the present study, further experiments in mouse models of cancer were done with two groups of bacteria: those containing the long form of the CDD gene and those in which the gene had been knocked out. Only the group with the CDD gene intact exhibited resistance when the drug was given to the mice. After treatment with antibiotics, this group also responded to the chemotherapy drug.
SEE ALSO: Nanotech Drug Delivery Method For Cancer Could Replace Conventional Chemotherapy
The researchers are now examining whether bacteria are found in other cancer types and, if so, what effects they might have on the cancer and its sensitivity to other anti-cancer drugs, including a novel family of immune-mediated anti-cancer drugs.

Mice were used to demonstrate how treatment with antibiotics, on top of chemotherapy, may be significantly superior to treatment with chemotherapy alone. Photo by NanoRobotics Laboratory, Polytechnique Montreal / NIH
The research, which was conducted in Straussman’s lab, was led by his graduate student Leore Geller and conducted in collaboration with Dr. Todd Golub and Dr. Michal Barzily-Rokini of the Massachusetts Institute of Technology.
Photos: NanoRobotics Laboratory, Polytechnique Montreal / NIH
Related posts




Facebook comments